 In manufacturing, quality control (QC) is very important. A manufacturer always wants to put out the best product and eliminate defective merchandise.
In manufacturing, quality control (QC) is very important. A manufacturer always wants to put out the best product and eliminate defective merchandise.
The same is true of IVF. With as many as 30 embryos created for every live birth, doctors are always on the look out for ways to separate the robust embryos from the “defective” ones to improve their success rates. Previously this was achieved by preimplantation genetic diagnosis (PGD.) In PGD, a single cell is removed from the days old embryo and tested for genetic anomalies. The ones that pass the test get a chance at being transferred to their mother’s womb. The others…well they are defective so no need to mention what happens to them, right?
PGD is expensive and invasive to the embryo, so an IVF clinic in Britain has developed a new way to QC embryos: time-lapsed photography. Those embryos that reach a certain stage slower than their counterparts are deemed “high risk.” High risk means high risk for aneuploidy. Aneuploidy is when embryos have too many or too few chromosomes. High risk embryos, according to the authors of the study, did not implant at all.
From BBC News:
Time-lapse imaging which takes thousands of pictures of developing embryos can boost the success rate of IVF, according to British research.
The method, reported in Reproductive BioMedicine Online, can be used to select embryos at low risk of defects.
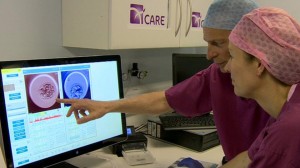
Scientists at the CARE fertility group say such informed selection can improve birth rates by 56%.
Other experts say the result is exciting, but the study of 69 couples is too small to be definitive.
The research followed the couples at the CARE fertility clinic in Manchester last year, when 88 embryos were imaged and implanted.
The embryos were put into an incubator and imaged every 10-20 minutes.
The researchers classified the embryos as low, medium or high risk of chromosome abnormalities based on their development at certain key points.
Eleven babies were born from the low risk group (61% success rate) compared to five from the medium risk group (19% success rate) and none from those deemed high risk.
“In the 35 years I have been in this field this is probably the most exciting and significant development that can be of value to all patients seeking IVF,” said Prof Simon Fishel, managing director of CARE Fertility Group.
“This technology can tell us which embryo is the most viable and has the highest potential to deliver a live birth – it will have huge potential. This is almost like having the embryo in the womb with a camera on them.”
But it isn’t anything like the womb; evidenced by the fact that a camera is watching your every cell division. Using this technique, clinics will identify the “low risk” embryos and discard the “high risk” embryos. That is called quality control, my friend.
And one of the conditions that will likely be called “high risk” because of the extra chromosome 21, is Down Syndrome. Quality control in human manufacturing has another name. It is called eugenics.
You may think I am being harsh comparing this new technique to manufacturing QC. That is until you read this comment by the chair of the British Fertility Society:
Allan Pacey, lecturer in andrology at Sheffield University and chair of the British Fertility Society, said: “This paper is interesting because we really do need to make advances in selecting the best embryos created during IVF.”
Mass produce, screen the product, choose the best and cull the rest. Above all, NEVER mention that these are actual human beings.



